My first big foray into research was the HETI sponsored project into rural ambulance utilisation. We know anecdotally that rural hospitals have high self-presentation rates and many rural paramedics have stories of the farmer who appeared in the ED ambulance bay with a major multi trauma having bounced down miles of country road in a ute with no treatment whatsoever. This posed a number of interesting questions. The principal question was “how often does this happen?” This is an interesting because previously noone had looked at an ambulance service’s “market share” of sick people. We measure well what ambulance services do but rarely compare it to the pool of potential patients.
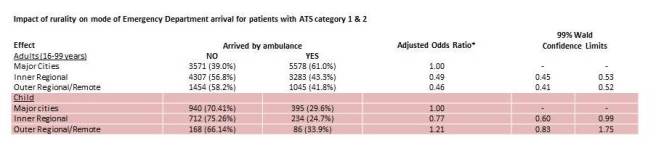
To find out we looked at a year’s worth of ED data from an Area Health Service with both urban and rural areas. Rurality was defined by the Australian Standard Geographical Classification. From this data we separated patients who arrived by ambulance from those who arrived by other means. We principally stratified by acuity based on the Australasian Triage Scale but also analysed against age, gender, aboriginality, and a range of other factors. A retrospective analysis of 354,746 ED cases found that the proportion of ambulance use for both high acuity patients (as defined by a triage score of 1 or 2 in the Australiasian Triage Scale) and across the general patient population to be lower in more remote locations than in metropolitan locations. This analysis found that six in every ten rural patients with serious health emergencies arrived by a mode of transport other than ambulance.
Jason Bendall and I found that rurality was a predictor of ambulance usage in almost all category of patient. There was no significant difference in age or gender although it was noted that children under three were significantly more likely to be transported by a means other than ambulance even in life threatening situations. While one of the limitations was that we could not separate interhospital transfers from primary ambulance transports, we did find they constituted only a small percentage of hopsital patient arrivals.
Other studies have found similar discrepancies between rural and urban areas. In a study by Brismar, Dahlgren and Larsson (1984) urban usage was almost double rural usage in analysis of two regions in Sweden. This study also outlines the differences in the character of rural and urban workload. Also from Scandinavia, Beillon, Suserud, Karlberg and Herlitz (2009) found that not only was use lower but acuity was often higher in rural patients. Unfortunately most work around ambulance demand is focused around inappropriate use rather than utilisation analysis.
Several other questions arose from the study including why rural people make decisions to transport other than by ambulance, whether ambulances actually good for you (ie will the presence of an ambulance change your clinical outcome versus self transport), and whatt steps can be taken to increase ambulance use in rural populations experiencing health emergencies. I will look at these in future blog posts.
You can read the full report here.